NEW DELHI — When the Indian Council of Medical Research (ICMR) invited quotes for millions of rapid diagnostic kits in the last of week of March this year to quickly test for COVID-19 antibodies, BioMedomics submitted a quote and noted the difficulties of delivering such a large number of kits at short notice.
The caveat was important: BioMedomics, an American firm with a manufacturing facility in China, was one of the first companies in the world to produce such test kits. They had developed their kit in late February and were already exporting these tests to the middle east and southeast Asia, so had experience with the complexities of manufacturing and shipping in the midst of a global pandemic.
When ICMR issued procurement letters on March 27 and March 28 to vendors who had won the bid — BioMedomics was not one of them. But documents reviewed by HuffPost India reveal ICMR had ordered 500,000 BioMedomics tests from a distributor who wasn’t authorised to sell these kits. BioMedomics complained to ICMR on April 4, but never heard back from the agency, according to a company representative.
In their letter, BioMedomics asked ICMR to cancel the purchase order, noting that “the party that quoted for our product does not represent the company in India nor does it have any commercial relationship with the company.” The company does “NOT take any responsibility for the quality or performance of the test kits supplied through this PO.”
The company confirmed to HuffPost India that BioMedomics never supplied these 500,000 kits to ICMR — neither directly, nor via a third-party distributor.
The rest of the order fell apart as well: ICMR had ordered tests from Indian distributors for two Chinese firms Zhuhai Livzon Diagnostics Inc and Guangzhou Wondfo Biotech. The kits arrived well after their designated date, and state governments soon claimed the tests were failing to deliver results. A commercial dispute between Wondfo’s India distributors revealed ICMR had agreed to pay Rs 600 for tests that cost only Rs 245 — leaving a distributor margin of 145%.
On April 27, a month after the tender was first announced, ICMR directed state governments not to use this particular consignment of rapid diagnostic kits, and announced it would not pay for them.
India’s punitive national lockdown, which has brought millions of vulnerable Indians to the brink of destitution since it was first announced on March 24 this year, was supposed to buy valuable time to establish the widespread testing infrastructure that, experts around the world agree, is a prerequisite to reopen the country.
Yet interviews with experts, state government officials, test manufacturers and distributors, and reviews of tenders, news reports and public statements indicate that ICMR, the agency tasked with leading India’s testing efforts, has wasted this hard-won window of time, raising uncomfortable questions over Prime Minister Narendra Modi’s handling of the on-going crisis.
“The delays in procurement are happening in a background of relatively low levels of testing overall,” said Gautam Menon, a professor of physics and biology at Ashoka University. “Without broad-based testing, we will simply have no idea of where and to what extent the disease has spread. This will make planning for opening up in a post-lockdown scenario that much more difficult.”
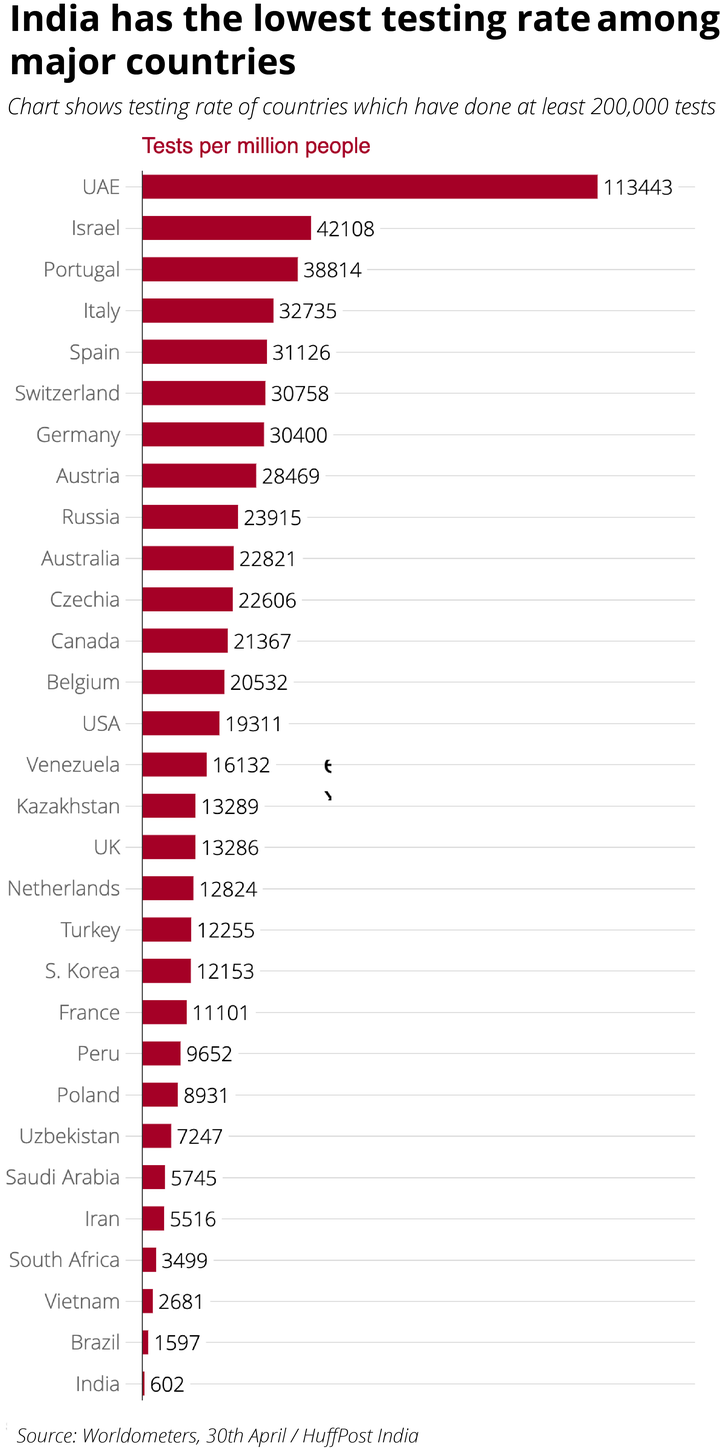
ICMR was tasked with scaling up coronavirus tests as early as February 3 2020; two months later, it is clear the agency has failed its mandate. As of date, India has tested a fraction of its 1.3 billion strong population. Among the 133 countries that have reported at least 100 cases, only 18 countries have a lower testing rate than India. In fact, the United States — a country synonymous with inefficient testing — has tested seven times more people than India despite having one-fourth the population.
Part of the reason, state health officials say, is that ICMR is a research organisation — not a procurement agency with the experience necessary to manage global tenders in a cutthroat market.
“Procurement is a specialised job. You need people who can read documents of import licenses, drug licenses,” said a senior officer in the Chhattisgarh government. “ICMR is not competent to do that. They are good for scientific work. But they are pathetic at procurement.”
Worse, the Modi government has prevaricated over exactly who — state or centre — is responsible for procuring vital supplies to tackle the novel coronavirus pandemic. Rather than helping capacity-strapped state governments by quickly setting standards and establishing benchmark prices, state health officials from Andhra Pradesh and Chhattisgarh say, the union Ministry for Health and Family Welfare’s lack of transparency, penchant for centralisation, and outright confusion, has made it harder to do their jobs.
Rather than leveraging India’s giant population to drive down prices, ICMR has sowed confusion that has forced state governments to bid against each other for scarce testing kits.
“The central government should play a good role in facilitating an ecosystem. But instead of facilitator, you want to become controllers,” the Chhattisgarh government official said, explaining that till as late as last week of March, state health departments were led to believe that ICMR would provide them with sufficient test kits. As medical supplies didn’t arrive as promised, the official said, a few state governments decided to procure test kits themselves.
Yet rather than own up to its failures, ICMR has retreated into obfuscation, denial and silence. In public statements, union health ministry officials trot out statistics on the number of tests ordered and tenders released, rather than reveal just how many of these orders and tenders have been fulfilled.
As of date, tenders, news reports and public statements by ICMR officials suggest ICMR has floated tenders for at least 6.5 million rapid diagnostic kits since March 2020 — of which, the only kits that seem to have arrived is the ill-fated consignment of 500,000 Chinese kits that ICMR refused to pay for.
The manufacturers deny the kits are faulty. Wondfo has pointed out it was the first antibody test kit to be validated and approved by ICMR through the National Institute of Virology, Pune, on 27th March.
ICMR did not respond to HuffPost India’s requests for comment.
Procurement problems
The global spread of the novel coronavirus has resulted in a worldwide shortage of medical supplies as countries rush to outbid each other in a scramble to stockpile everything from testing kits and protective gear, to facemasks and cleaning products.
This supply crunch, suppliers, manufacturers and government officials say, favours countries with efficient, well-thought, procurement strategies — making the Indian government’s decision to let ICMR handle procurement puzzling.
“There is no shortage of kits,” said Ujjwal Handa, the director of AnjanaJyoti Systems which is importing South Korean test kits. “We can deliver one million tests in seven days.”
But manufacturers reserve their inventory for buyers who pay upfront, Handa explained.
ICMR’s tenders make clear that the agency will only pay for kits upon delivery; creating an opening for importers — or middlemen — who risk paying the manufacturers upfront in the hope that ICMR will clear their shipments and pay for their tests. But importers add hefty margins to the price of the kits to compensate for the risk that the ICMR could reject the order without paying, industry observers said.
This trade-off between low-prices upfront versus high prices upon delayed payment was visible in a recent Delhi High Court case involving the first batch of 550,000 rapid kits that arrived in India from China on 16th April. The Wondfo kit procured by importer Matrix Labs for Rs 245 was eventually sold to the government at a 145% mark-up for Rs 600—with another distributor in between. Once the case came to light, ICMR cancelled the order without paying the importers, claiming the kits didn’t work.
“Because of the due process followed (not going for procurement with 100% advance amount), GoI does not stand to lose a single rupee,” the Ministry of Health and Family Welfare said in a press release.
“ICMR didn’t lose a rupee but didn’t gain anything. And also lost valuable time,” a Delhi-based kit importer said on the Chinese kits fiasco.
The payment terms aren’t the only problem.
“The contract penalises us if the shipment is delayed. But how can we promise a date until we know when the order will be finalised and some payment will be made,” a South Korean supplier told HuffPost India, adding that the international movement barriers sometimes lead to unexpected delays not in the supplier’s control. “Why should we be penalised for this? That’s why it has been very stressful in applying for contracts in India.”
Chhattisgarh And Andhra Pradesh
Where ICMR has struggled, some state governments have proved to be much better at securing supplies of coronavirus test kits.
On April 17, Chhattisgarh health minister TS Singh Deo tweeted that the state had ordered 75,000 rapid tests directly from South Korean company SD Biosensor at Rs 337 per kit. The kits are being manufactured in BioSensor’s plant in Manesar, Haryana and the first batch of 25,000 tests have already been delivered to the Chhattisgarh government.
Procuring directly from the manufacturer, and that too from a domestic factory, has resulted in much lower costs and fewer logistical challenges, an advisor to the Chhattisgarh government said.
Chhattisgarh did not pay for the BioSensor kits in advance, the senior state government officer quoted earlier in the piece confirmed. Manufacturers are willing to supply to governments without an advance, the officer said, “but they need to know what is the government’s intention.”
A firm assurance of timely payment, the officer said, goes a long way. Chhattisgarh’s lower price unexpectedly worked to the benefit of the neighbouring state of Andhra Pradesh. Andhra Pradesh had ordered SD Biosensor kits as well, except at Rs 730 per kit through an importer authorised by the company.
“The market was dicey at that time and prices being quoted by companies varied a lot,” said V Vijaya Rama Raju, Vice Chairman and Managing Director of Andhra Pradesh Medical Services and Infrastructure Development Corporation, the agency tasked with procuring tests for the AP government. Raju explained that the state government agreed to a higher price as they anticipated shortages in the market.
“We put in a safety clause in the contract stating if the kits are bought at a lower price by any state government, that price will apply to AP too,” Raju said.
The day after Chhattisgarh made its procurement price public, Raju said he wrote to SD Biosensor. The safety clause in the contract meant Biosensor quickly agreed to produce test kits to AP at the same low price as Chhattisgarh.
“Usually, this huge price difference would not have happened because the states would have been in touch with one another to find out the rates offered different companies,” said an Andhra Pradesh health official. “But during the lockdown each of the states were left to battle for themselves and not many procurement agencies were in touch with one another.”
The Chhattisgarh official agreed.
“At this time, most states are not interacting and working in silos,” the officer said. “They are afraid to share data with other states.”
In theory, a nodal agency like the ICMR could have coordinated with states to prevent them from bidding against each other. In practice, the agency has sowed uncertainty and confusion that has scared off genuine suppliers and left state governments in a lurch.