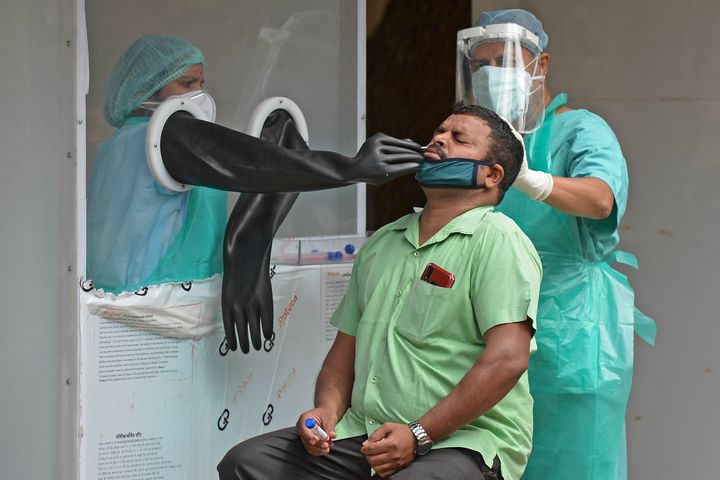
With no clinical diagnosis protocols in place to detect the presence of COVID-19 infection in a person, RT-PCR testing is considered the most reliable test in India. However, a lack of attention to quality control has resulted in “misleading” results, says T. Jacob John, a retired Professor of Clinical Virology, CMC, Vellore and former president of the Indian Academy of Pediatrics.
“We do not have clear clinical diagnosis protocols in place to assess the reliability of the lab results. The blind faith in laboratories and in PCR tests have misled the government to underestimate the real extent of the pandemic spread in the country,” he said in an interview.
John also said that if Indian doctors were taught to diagnose Covid-19 infections clinically before using PCR tests to confirm it, test positivity rates would rise and costs would be lower.
Edited excerpts:
What is RT-PCR testing and how is it done in India?
Every infectious disease has its causative microbe and the names of the microbe and the disease are semantically linked. In this case, the microbe is SARS Coronavirus type 2 (SARS-CoV-2) and the disease is Coronavirus disease 2019 (COVID-19).
In many situations, a lab test is resorted to in order to ‘diagnose’ infection, which in turn supports the ‘diagnosis’ of disease. Although TB and AIDS could be clinically diagnosed with clinical diagnostic criteria, to be absolutely sure of the diagnosis, a sputum smear test is applied to visualise the TB bacilli and an HIV antibody test is used to confirm if the person is infected by HIV.
For COVID-19, a typical case does not require a lab test but for epidemiological purposes, in order to quarantine or hospitalise the person, a lab test to confirm infection is used—in our case, ‘reverse transcription polymerase chain reaction’ test (RT-PCR test).
What the test detects is a small segment of the viral genome, a segment that is present only in SARS-CoV-2 and not in any other coronavirus. So, if the gene segment was present in the nasopharyngeal swab, then we know the virus was present, and the person is infected. If the person has no disease symptoms, he/she is infected but without disease ― asymptomatic infection, in other words. During contact tracing and testing, most test-positives are asymptomatic infections.
Reverse transcriptase enzyme synthesises DNA complementary to the RNA segment. Then DNA is copied continuously, 1 becomes 2, then 4, and 8 and so on in a “chain reaction”. When sufficient numbers are reached, they can be detected.

RT-PCR tests are considered to be the gold standard of testing for the novel coronavirus. How reliable are they? What are some common reasons why these tests might show false positives or false negatives?
The validity of an RT-PCR testing depends upon the laboratory quality and its meticulous attention to the protocol prescribed for processing a test sample. But unfortunately, the selection of private labs in India has not been done carefully. Apart from the chances of cross-contamination in the lab, the way samples are being collected too have resulted in misleading results. For example, various studies have shown that since the viral load in the throat would be less than in the nasopharynx, the throat swabs have resulted in over 60% false negative results, while nasal swabs have resulted in only 30% false negative reports. False positive results happen only in labs not following protocol very strictly. So false positive results are far fewer than false negative. Even today, we do not have any mechanism to check the number of false positives and negatives coming from various labs, especially in asymptomatic people in India.
ICMR has authorised private testing labs to conduct RT-PCR testing in India but many have handed over testing kits to private hospitals to take the specimen and transport them to labs. Do you think that this protocol of SARS COV-2 sample testing in India is in accordance with ICMR guidelines or has testing been compromised in India?
In India, RT-PCR testing remains the most popular method to identify coronavirus positive persons. We do not have clear clinical diagnosis protocols in place to assess the reliability of the lab results. The blind faith in laboratories and in PCR tests has misled the government to underestimate the real extent of the pandemic spread in the country. Many media reports have highlighted how false ‘positive’ results have been identified in various labs. If a person with false positive results is quarantined with true positive persons, the former will be exposed to infection and may even get infected.
The medical team should alert the authorities in case of a suspected false positive result and should get re-testing done in another reliable lab. . If discrepancy is noted, the first laboratory must be closed and re-checked for quality assurance with compliance with protocols and record-keeping.
What is the best testing sample for SARS COV-2? Do you think that our testing is accurate? Since health is a state subject, do you think that the state governments are holding stringent checks to safeguard the identity and sanctity of the testing samples collected in private hospitals?
Standardisation and quality assurance of lab tests have been a problem for a long time in India. Every lab must participate in a national external quality assessment scheme by testing and reporting coded samples sent from a reference lab. CMC Vellore’s Virology Department supplies blinded samples for external quality assessment, under the aegis of Indian Association of Medical Microbiologists. Participation is voluntary. Another quality certifying process is accreditation. National Accreditation Board for [Testing and Calibration] Labs will accredit diagnostic labs after quality assurance.
In a recent article written in The Hindu, you have called RT-PCR testing a double-edged sword. Can you elaborate on this a little?
As I said earlier, the plus and the minus of PCR testing are in its capacity to amplify even one viral gene segment in the sample. Thus it is a very good test, when positive, in a quality-assured lab. But even in the best lab, the test is prone to false negative results.
PCR is done on deep nasal (nasopharyngeal) swab and/or throat swab. The throat carries less viral load than deep nasal mucous membrane. So, a throat swab may not have picked up the virus, in which case the result will be falsely negative. More than 50% throat swabs may be falsely negative. Deep nasal swabs are better but even with that about a quarter may be falsely negative. If one throat and one deep nasal swab are put in one specimen collection tube, the probability of true positive result increases.
Are you satisfied with India’s testing regime? Are we testing as widely and as often as you would like?
I had better not give an opinion since there have been several directives and each state follows its own testing strategy, broadly aligning with ICMR instructions. I am not happy that doctors have not been taught clinical diagnosis of Covid using clinical criteria and then using PCR to confirm clinical diagnosis by detecting infection. If that is done, our test positive rate will be much higher and we would have reduced expenses per detected infection. Testing for contact tracing went on far too long, which is why the government kept on denying community transmission.
In the absence of a culture of appropriate use and availability of labs in government healthcare institutions, even in many district hospitals, ad hoc arrangements had to be made, with many labs authorised to test, but the government has hardly any system for quality checks.
ICMR initially set August 15 as the deadline for the development of a vaccine for coronavirus, before backtracking on the date. What is your take on this?
I think the wording was to complete studies in order to launch a vaccine by that date. That is simply not possible. Phase 1 and phase 2 of the vaccine trial will take at least about 5 months. Only after both phases are completed and the candidate vaccine certified as both safe and effective in inducing immune response can phase 3 part start. Phase 3 is to see if the immunity stimulated by the vaccine protects from disease when exposed. Phase 3 will require another 3-6 months, depending upon the number of cases in the placebo arm of the phase 3 trial. So, altogether 8-11 months will be the minimum time required before we know if we have a vaccine or not.